By Izzy D’Alo and Caroline Leland
 “How can we adapt our practices so they do not re-traumatize someone?” Thorp Faculty Engaged Scholar Jessica Williams, an assistant professor at the UNC-Chapel Hill School of Nursing, is working on developing and implementing community-informed answers to this big question.
“How can we adapt our practices so they do not re-traumatize someone?” Thorp Faculty Engaged Scholar Jessica Williams, an assistant professor at the UNC-Chapel Hill School of Nursing, is working on developing and implementing community-informed answers to this big question.
Although 25 percent of women experience intimate partner violence (IPV), Williams has observed that many health care practitioners are not trained to identify trauma as a cause for chronic conditions, nor are they trained for situations where a patient discloses trauma.
“Oftentimes when we address issues of abuse, we address it from a social services or criminal justice perspective. We (tend to) focus on it much less from a health perspective,” Williams said. She points to chronic pain and substance use as examples of health challenges that can be linked to past or ongoing trauma, including emotional trauma.
“We treat symptoms of pain,” she said. “We aren’t really thinking about what might be the root cause of the pain.”
Williams also noted that certain health care practices may be triggering for victims, especially if a provider is not trained in trauma-informed care. For example, childhood trauma sometimes causes post-traumatic stress disorder that can affect how a patient reacts to or feels about the health care system. It’s important for providers to understand how factors like these can affect a patient’s experience.
To address challenges like these, Williams facilitates trainings for health care providers and domestic violence resource centers. Her current work is primarily centered in a partnership between the North Carolina Coalition Against Domestic Violence and North Carolina Community Health Center Association. These organizations work together to strengthen relationships between health providers and IPV service agencies through grants funded by Futures Without Violence and Blue Cross and Blue Shield of North Carolina Foundation. As a Thorp Faculty Engaged Scholar (FES), Williams helps to inform the projects made possible through these grants.

“Where the Thorp program was instrumental was that it helped identify what are the barriers,” Williams said. Using funding from FES, Williams organized a community forum with key stakeholders: staff advocates for domestic violence service agencies, policymakers, survivors and others. This forum helped Williams and her partners to identify strengths and opportunities inherent in partnerships between health care organizations and IPV service agencies, enabling them to form a strategy for facilitating the partnerships and educational trainings that stem from those partnerships. The forum also helped Williams identify specific health needs of IPV survivors.
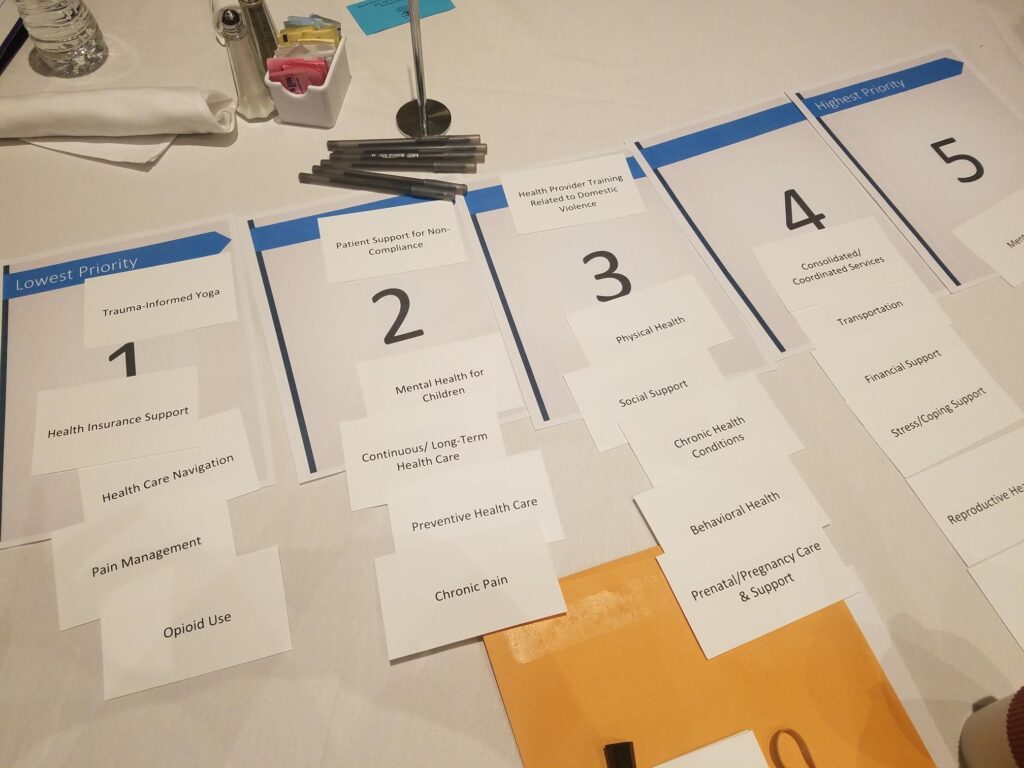
As a result, the NC Coalition Against Domestic Violence has begun trainings across the state for doctors and other health care professionals to make the health care environment more welcoming and safe for victims of IPV.
Williams said the interdisciplinary nature of FES helped make her work possible.
“The cohort of scholars has been helpful. The funding is nice, but I think the most valuable part is being able to collaborate with other scholars and learn from their work, their challenges and their successes,” she said. “Even though we’re all in different areas, different schools — there’s so much overlap.”
Williams’ work continues to illustrate that same collaborative mindset.
“Experiences of abuse are not just a social problem, a criminal justice problem, a health problem. It’s all of those things,” she said. “It takes a community to address those issues. We’re not going to see the issue of abuse and violence effectively addressed until we take that collaborative approach to addressing it.”
